Table of Contents
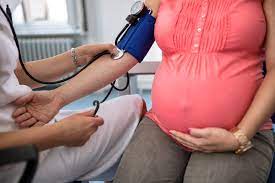
Hypertension during pregnancy, commonly referred to as pregnancy-induced hypertension (PIH) or gestational hypertension, is a significant medical concern affecting expectant mothers.
Contrary to most beliefs that hypertension can only be caused by stress, alcohol consumption, hard drugs etc, pregnancy has also been proven to cause hypertension. So women develop high blood pressure for being just pregnant. Most times the patient can become normotensive after given birth, but in some cases, the blood pressure remains high even after childbirth.
Pregnancy-induced hypertension is based on the appearance of high blood pressure ≥ 140/90mm/Hg after 20 weeks of gestation with proteinuria (protein in the urine) and oedema (swollen parts of the body due to fluid accumulation). Pregnancy-induced hypertension is also known as Pre-eclampsia.
Gestational hypertension is also another type of pregnancy-induced hypertension but it differs from Pre-eclampsia based on its major symptoms.
PRE-ECLAMPSIA
- High blood pressure
- Oedema
- Proteinuria (Characterized by frothy urine(foamy urine))
GESTATIONAL HYPERTENSION
- High blood pressure
- No proteinuria
- No oedema
But both of them are induced by pregnancy.
PREVENTION OF PRE-ECLAMPSIA
One of the most used prophylactic agent(preventive) for the development of any hypertension at all is low dose aspirin, usually 60mg. Aspirin is an antithrombin agent. It prevents the release of thrombocytes from the platelets. Since thrombocytes are known hypertensive agents, aspirin reduced the risk of developing hypertension, and it can also be used in the case of pregnancy. Under the supervision of a certified health practitioner, pregnant patients can use aspirin to prevent the development of Pre-eclampsia.
Proper antenatal care cannot be overemphasized. Pregnant patients should always go to the hospital for a total check-up, not just for the foetus but also for the mother. Antenatal appointments would help to discover if a patient is at risk of developing pre-eclampsia, and also helps to monitor patients who developed pre-eclampsia in previous pregnancies.
EFFECTS OF PRE-ECLAMPSIA
- Birth defects: Structural defects in the child has been seen. During pre-eclampsia, required nutrients do not get to the foetus, if the baby survives the baby might have a birth defect, such as reduced height, and body weight.
- Reduction in the flow of required nutrients to the foetus through the placenta.
- Placenta insufficiency
- Development of comorbidities in the foetus and the mother: Hypertension is both a disease and risk factor. As a risk factor, it can induce diabetes, kidney failure, liver failure, nephropathy, neuropathy and retinopathy, both in the mother and foetus.
- Improper development of the foetus.
DRUG TREATMENT IN PRE-ECLAMPSIA
Not all anti-hypertensives are to be used in pre-eclampsia, as some anti-hypertensives could be harmful to the foetus. Usually, centrally acting hypertensives can be used. Examples are:
Alpha methyldopa: It reduces sympathetic drive. Activation of the sympathetic system results in hypertension, alpha methyldopa prevents this from happening. Side effects include headache, nightmares, asthenia.
Hydralazine (A vasodilator): Hydralazine a vasodilator, causes an increase in the release of nitric oxide. Nitric oxide causes vasodilation of the blood vessels. This leads to a reduction in blood pressure. Side effects include flushing, nausea, vomiting, tachycardia.
Channel blockers (E.g Nifedipine): Influx of calcium, through Calcium gated voltage channels, leads to an increase in blood pressure. Nifedipine blocks these channels preventing the influx of calcium, thus reducing the blood pressure. Side effects Nausea, vomiting, flushing.
Magnesium sulphate: In pregnancy-induced hypertension, it isn’t given for Hypertension, it is given to prolong pregnancy and improve the development of the foetal lungs, but it has been shown to reduce blood pressure.
For individualization of therapy, so that optimum results can be established, each patient should talk directly with a health practitioner for the dose to be individualized for her.
AIMS OF THERAPY
- To reduce cardiovascular complications such as myocardial infarction, ischemia.
- To reduce the development of neuropathy in both the foetus and mother.
- To improve the chances of having of normal foetal outcome.
- To reduce chances of developing kidney failure.
- To reduce the development of nephrotic syndrome, which reduces the chances of formation of frothy urine.
ALSO READ:
Boosting Your Odds of Having Twins: 7 Effective Tips
7 Factors Behind the Aba Women’s Riot of 1929
6 Strategies for Recognizing Prideful Behaviors
How to get a Job during School Holidays
Leave a Reply